What Is a Coronectomy? A Complete Guide to This Wisdom Tooth-Saving Procedure
A coronectomy is a dental procedure in which the top or the wisdom tooth crown is extracted, and the roots are retained at their current location, by being securely embedded in your jaw. It also sounds very strange, doesn’t it? And like ordering a burger and just biting the bun. It is perfectly logical, however, once you see the reason why it is done.
This isn’t a common procedure; it’s a very specific solution for a very specific situation. It is done when the roots of a wisdom tooth are too close to the inferior alveolar nerve, which is the primary nerve that runs through your lower jaw. When that nerve is interfered with in a normal extraction, you may have numbness or tingling in your lower lip and chin, and it may last months, sometimes forever. A coronectomy does not do that at all.
Like many other dental conditions that seem alarming on paper but are very manageable with the right approach, a coronectomy is one of those procedures that patients usually leave feeling relieved, not stressed. If your dentist has recommended one, this guide walks through everything: what it involves, what recovery really looks like, whether it’s more painful than a regular extraction, and what happens to that root long term.
Quick Fact
A coronectomy is the intentional removal of a wisdom tooth crown while leaving the roots in place (in situ) to protect the inferior alveolar nerve. It is recommended when imaging confirms high-risk contact between the root and the nerve canal.
Why Would a Dentist Recommend a Coronectomy Instead of Just Pulling the Tooth?
The point is that most of the wisdom teeth are removed without any complications. It is just a usual practice. There are other wisdom teeth. Their roots are curled, grow at strange angles or even directly over a very sensitive nerve in the jaw. Once that occurs, extracting the entire tooth in one quicker movement is now that much more dangerous than it should be.
This nerve is known as the inferior alveolar nerve (IAN). It takes care of the sensation in your lower teeth, your lower lip and part of your chin. Should it be damaged in an extraction, it may result in numbness, burning, or a tingling sensation that, in certain cases, may not be resolved. That is no trifle. It influences your drinking, talking, and touching your face.
A coronectomy removes the crown, the part that hurts, gets infected, or causes crowding, and leaves the roots untouched. The nerve stays safe. The problem tooth is gone. That’s the trade-off, and for patients where the imaging shows genuine risk, it’s absolutely the right call. Our oral surgery team at Al Dental Studio makes this decision based on detailed 3D imaging, not guesswork.
Studies show that inferior alveolar nerve injury occurs in roughly 0.4% to 8.4% of standard wisdom tooth extractions. But in high-risk cases, where the roots are directly in contact with the nerve canal,, that number climbs sharply. A coronectomy dramatically lowers it. That’s why this option exists, and why it’s taken seriously by oral surgeons who look at the full picture before deciding.
Quick Fact
Research published in the British Journal of Oral and Maxillofacial Surgery found that coronectomy carries a permanent nerve injury rate of less than 1%, compared to significantly higher rates in high-risk full extractions, making it the evidence-backed safer option in appropriate cases.
Here's What We See at Al Dental Studio: How Do We Know If a Coronectomy Is Right for You?
Not every wisdom tooth needs this procedure; that’s important to say upfront. The decision starts with imaging. A standard panoramic X-ray can give us early clues: roots that look darker near the nerve, roots that appear to narrow at the point where they cross the nerve canal, or roots that seem to ‘disappear’ into the nerve. These are the flags we look for.
When those warning signs show up, we follow up with a cone beam CT scan, essentially a 3D map of the jaw. That scan tells us exactly how close the roots are to the nerve, and in some cases, we can see the nerve canal running directly through the root itself. At that point, a coronectomy isn’t just an option; it’s the responsible recommendation.
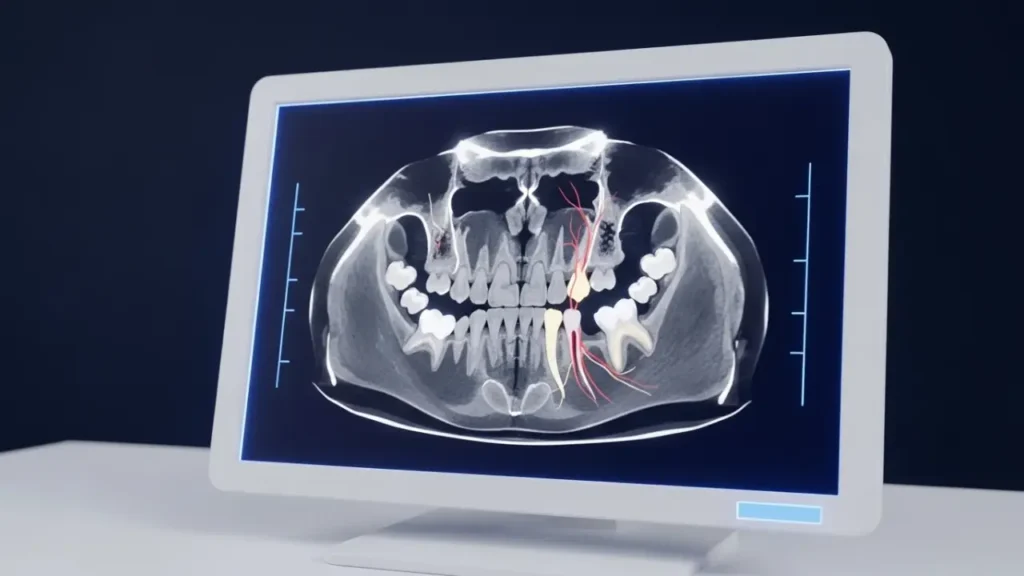

Patients in their 20s and early 30s are most likely to land in this situation. That’s when wisdom teeth have fully formed, and roots are at their longest, increasing the chance of nerve proximity. The good news: catching this early, before the tooth becomes a serious problem, means we can plan the procedure calmly, no emergency, no panic, just a clear and safe plan.
If your dentist flagged your wisdom tooth and mentioned a nerve, don’t worry. That flag isn’t a sign that something went wrong; it’s a sign your dental team is paying close attention. That’s exactly what you want from an oral surgeon.
Step-by-Step: What Actually Happens During a Coronectomy Procedure?
Patients are often surprised to find out how similar a coronectomy feels to a regular tooth removal. You won’t feel any cutting or drilling, just the occasional pressure or vibration, and only because the local anaesthetic has already done its job. Here’s the full breakdown of how it goes.

Step 1: Detailed Imaging Review (Before You Even Sit Down)
Your oral surgeon or dentist reviews your panoramic X-ray and cone beam CT scan before the appointment. They are tracing the precise location of the crown, the location of the nerve, and the amount of tooth tissue which must be removed. It is this pre-planning that makes the process accurate; no calculations are made at the hour of need.
Step 2: Local Anaesthesia
To ensure that the area is numb, a local anaesthetic injection is given in the lower jaw. The majority of patients experience a small pinch; a few hardly feel it. Within a few minutes, the whole area is numb, and you won’t feel a thing from that point on. Request about nitrous oxide (laughing gas) in case you are nervous. It is there, and it does make a difference.
Step 3: Removing the Crown
The dentist takes the time to cut and extract the crown of the wisdom tooth. It is done by lifting the gum tissue softly in order to reach it. After the crown is removed, the remaining root surface is made smooth by the dentist, which creates a flat and comfortable position of the gum line. Nor are there any jagged edges, no root jutting out.
Step 4: Closing the Site
Stitches are made on the gum tissue to seal the root with dissolvable sutures. These dissolve by themselves; no second visit to get stitches taken out. The area is covered and enclosed, and recovery begins immediately.
Step 5: Leaving with a Clear Plan
The team, before you go, takes you on a tour of what you need to eat, what to avoid and what to watch in the days to come. The entire process typically requires 30-60 minutes between the initial injection and the final stitch. The majority of patients are self-driving and, within an hour, are seated on the couch watching TV.
What Does Recovery Actually Look Like? The Week-by-Week Timeline
Recovery from a coronectomy is usually easier than patients expect. It’s similar to a standard wisdom tooth removal, some soreness, a little swelling, a few days of soft food, but without the open socket that tends to make standard extractions a bit more involved.


| Timeline | What to Expect |
|---|---|
| Day 1–2 | Some bleeding, mild swelling, and soreness. Rest is the priority. Soft foods only (yoghurt, mashed potatoes, smoothies). Apply an ice pack (20 minutes on, 20 minutes off). Take pain relief as directed. |
| Day 3–4 | Swelling peaks around day 3 and then starts to go down. Pain reduces noticeably. Keep the area clean—gentle warm salt-water rinses help. Avoid heavy chewing. |
| Day 5–7 | Most patients feel significantly better. Eating becomes more comfortable. Swelling has mostly settled. You’ll look and feel almost normal. |
| Week 2 | Back to everyday activities. Mild tenderness is normal. Avoid crunchy or hard foods. The site is still healing underneath. |
| Week 3–4 | Fully healed for most patients. A follow-up X-ray may be scheduled to check the root position and ensure proper healing. |
| Long-term | The retained root is monitored with periodic X-rays. In many cases, it gradually migrates away from the nerve over time. |
Everyone heals at a different pace; that’s just how it is. Some people are eating normally by day 5, others take closer to 10 days. The things that make the biggest difference: following your aftercare instructions, not smoking (it genuinely slows healing significantly), and contacting your dental team early if anything feels off.
Is a Coronectomy More Painful Than a Full Extraction? Here's the Honest Answer
This is the question we get most often. And honestly, the answer surprises people: for the majority of patients, a coronectomy is less painful than a full extraction, not more.
Think about it this way. In a standard extraction, the entire tooth comes out, roots and all. That means more force, more disruption to the bone socket, and a larger wound that needs to close and heal. In a coronectomy, the roots stay put. The bone around them doesn’t get disturbed. There’s no empty socket. The wound is smaller, healing is faster, and the body has significantly less to repair.
During the procedure, you won’t feel pain either way; the local anaesthetic takes care of that. After it wears off, you’ll feel soreness. That’s expected. But most coronectomy patients manage fine with standard ibuprofen or paracetamol. Stronger medication is sometimes prescribed for the first day or two, but most people don’t end up needing it beyond that.
There’s also the dry socket question. Dry socket is that sharp, throbbing jaw pain that can happen after a regular extraction when the blood clot shifts out of place. It’s genuinely unpleasant. After a coronectomy, the risk of dry socket is significantly lower because there’s no open socket to worry about. For anyone who’s had dry socket before and knows how bad it can be, that’s meaningful. For more on managing jaw pain and what’s normal vs. what isn’t after a procedure, that’s worth a read.
Coronectomy vs. Full Extraction: An Honest Side-by-Side Comparison
Here’s a direct comparison. A coronectomy isn’t the right choice for everyone; it’s a targeted procedure for a specific clinical need. Your dentist will be clear about which one applies to your situation.
| Feature | Coronectomy | Full Extraction |
|---|---|---|
| What’s removed | Crown only, root stays in | Entire tooth, root and all |
| Nerve damage risk | Very low, the root is kept away from the nerve | Higher if the root sits near or wraps around the nerve |
| Recovery time | 5–7 days for most patients | 7–10 days typically |
| Pain level | Mild to moderate, manageable with OTC meds | Moderate, similar or slightly more |
| Root left behind | Yes, intentionally | No |
| Dry socket risk | Lower, no open socket | Slightly higher |
| Long-term root behaviour | Root often migrates away from the nerve over time | Not applicable |
| Best suited for | Wisdom teeth near the inferior alveolar nerve | Most standard wisdom tooth removals |
Long-Term Outlook: Does That Root Just Sit There Forever?
This is a completely reasonable question. You leave the clinic knowing there’s still a piece of tooth in your jaw, of course, you want to know what happens to it. The answer is more reassuring than most people expect.
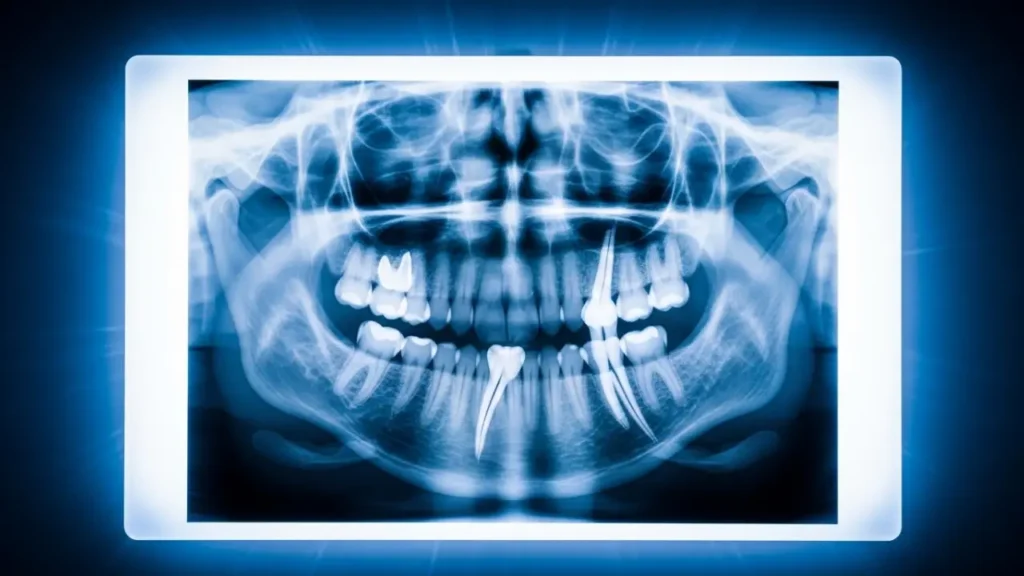

In the vast majority of cases, the root stays put and causes absolutely no problems. It gets covered over by bone and gum tissue as healing progresses. After a few weeks, most patients forget it’s even there. It doesn’t hurt, it doesn’t shift noticeably, and it doesn’t interfere with anything.
Here’s the part that actually surprises people: research shows that in a significant number of patients, somewhere between 33% and 58%, depending on the study, the retained root slowly migrates upward and away from the inferior alveolar nerve over the following 12 to 24 months. That’s a good outcome. It means the root that was once close to the nerve is now even further from it. Less risk, not more, over time.
Your dentist will keep an eye on things with periodic X-rays at follow-up visits. If the root ever does cause an issue, which is uncommon, it can be addressed at that point. But for most patients, it’s genuinely a non-issue after healing. Protecting your long-term oral health starts with getting the right procedure done the first time safely, and for high-risk wisdom teeth, that’s exactly what a coronectomy does.
Quick Fact
A 2019 review in the Journal of Oral and Maxillofacial Surgery confirmed root migration rates of 33%–58% in coronectomy patients over 24 months, with the root moving away from the inferior alveolar nerve canal, improving the long-term safety profile significantly.
Pain Management Before, During, and After Your Coronectomy
There’s not a lot to do before the procedure itself in terms of pain management. Turn up prepared and have a regular meal beforehand (unless instructed otherwise), and inform your team in advance whether you are nervous or not. Nitrous oxide exists and can relieve the entire experience of those patients who wish to have a bite.
The local anaesthetic takes care of everything throughout the procedure. You’re not going to feel cutting or drilling. Some pressure may be experienced when the tooth is being sectioned, but it is not painful. Consider it as being touched by a person on your arm and not on your hurt part.
The best thing after the procedure is to take your pain medication before the anaesthetic has completely subsided, not when you are already in pain. The packs of ice on the outside of your jaw in the first 24 hours (20-minutes on, 20-minutes off) are very helpful with swelling. Soft foods (yoghurt, smoothies and ice cream) that are cold in nature are also really good options on the first day and are soothing and easy to swallow, but not hot enough to have an impact on the healing site.
No straws, hot drinks, alcohol, or smoking for at least 48 hours. Straws cause suction that may cause disruption of the healing tissue. Smoking decreases blood flow and makes recuperation take a lot longer. They are not arbitrary rules; they are the things that will actually help make the difference between a smooth recovery and a rough one.
Frequently Asked Questions: Answered Directly
1. Is a coronectomy more painful than a full extraction?
For most patients, no, it’s actually less painful. The root stays in, so there’s less bone disruption and a smaller wound to heal. Soreness for a few days is normal. Most people manage fine with over-the-counter ibuprofen.
2. How long is the coronectomy recovery?
Most patients feel significantly better within 5 to 7 days. The first 48 hours are the most uncomfortable; after that, it improves noticeably. By day 4 or 5, most people are eating soft foods and going about their normal day.
3. What does coronectomy swelling look like, and when does it go away?
Swelling usually peaks around day 2 or 3, and it can look puffy around the jaw or cheek. Most of it settles by day 5 or 6. Applying ice in the first 24 hours makes a real difference. After that, the swelling resolves on its own.
4. Can the root be left in forever after a coronectomy?
In most cases, yes, and that’s the intended outcome. The root becomes covered by bone and tissue. It often migrates slightly away from the nerve over time, which actually improves things. Your dentist monitors it with follow-up X-rays.
5. How do I know if my coronectomy site is infected?
Watch for pain that gets worse after day 3 instead of better, a bad taste or smell, visible pus, or a fever. These aren’t normal and need attention quickly. Check our guide on warning signs of infection for more details on what to look for.
6. What is the success rate of coronectomy vs. wisdom tooth extraction?
Coronectomy has a success rate of around 95% or higher in appropriate cases. More importantly, it reduces permanent nerve injury risk dramatically compared to a full extraction where root-nerve contact is present.
For the infection question above, if you’re unsure what normal post-procedure discomfort looks like versus something that needs attention, our article on warning signs of infection and gum disease covers the red flags clearly.
So, Is a Coronectomy the Right Choice for You?
If your dentist has recommended a coronectomy, it means they’ve looked at your imaging carefully, weighed the risks, and decided that protecting your nerve is more important than removing every last piece of that tooth. That’s a thoughtful, evidence-based call, not a shortcut.
Most patients who go through a coronectomy are surprised by how manageable the whole thing is. The procedure is quicker than they expected. The recovery is easier than they feared. And the long-term result, a nerve that stays intact, a problem tooth that’s gone, and a root that quietly coexists with your jaw, is a genuinely good outcome.
You deserve to go into a procedure feeling informed and calm, not guessing. If you’re in NYC and wondering whether a coronectomy is right for you, or you’ve already been told it is and just want to talk through what to expect, our oral surgery team at Al Dental Studio is ready to walk through your specific case with you.
Wondering if a coronectomy is right for you? Contact our oral surgery team in NYC, and we’ll go through your imaging with you, explain exactly what we see, and give you a clear, honest recommendation.


Dr. Alexander Heifitz (DDS)
Dr. Alexander Heifitz is the founder of AL Dental Studio in NYC, where he combines advanced dental expertise with a patient-first approach. He specializes in cosmetic and restorative treatments such as dental implants, veneers, Invisalign, and smile makeovers, helping New Yorkers achieve both oral health and confidence.
Book An Appointment
Looking for a reliable dentist in Upper East NYC? Whether you need a routine cleaning, urgent care, or a full smile transformation, we’ve got you covered. We accept most PPO insurance plans and offer flexible scheduling.
+1 (212) 430-3888
Call for appointment
Walk-ins Welcome / Same-Day Appointments Available


Related Blogs

Causes & Treatments for Kids’ Cavities
Learn the main causes of cavities in children and explore effective treatments, from fluoride and fillings to proper oral care for healthy teeth.
Read More

15 Best and Worst Foods for Better Teeth (Dentist-Approved Guide)
Discover the 15 best and worst foods for better teeth. Learn which to eat and avoid for stronger, healthier, cavity-free teeth and gums!
Read More